
Strategic planning to reach diverse urology patients and broaden the user base
UX Design, Design Research
Time frame: 7 weeks
Client: Healthcare Company
Team members: Emmanuella Ben-Eboh, Sanhyong Park, Zixuan Zhao
Role: Strategic Designer, Researcher, UX Designer
Skills: Research Synthesis, Purpose Statement, Business Model Canvas, Strategic Roadmap, Wireframe, Prototyping, UX Design
How Might We Statement
How might we encourage prevention and treatment in early urologic patients without stigmatizing and requiring more effort from them?
Summary
Challenge
To expand business, the urology app needs to build a direct-to-patient sales model.
Our team worked on a challenge to create a new business opportunity for a client who was developing an urology diagnostic app. In the urology field, there are many potential patients, but many people are undiagnosed due to social taboos and lack of awareness. The challenge was to build a direct-to-consumer sales model to increase users and enable patients to diagnose at home, even in a pandemic.
Solution
Creating a urology community where diverse patients can easily participate.
We proposed building a urological information community targeting those who were concerned about their Lower Urinary Tract Symptoms (LUTS). Since there are many people with mild symptoms, we planned to use articles and blogs as a gateway to broaden the user base and build a community. From a simple diagnostic function, the app also proposes to users a behavioral change that leads to treatment. The revenue will be based on a freemium model, making it easy to adopt the app for users.
Research
We conducted secondary research and interviews to understand users and their current problems. Urology patients increase with age. They need a continuous diagnosis and want more efficient treatment. They also don’t talk much about their symptoms, so urology apps that are easily accessible at home could bring many benefits.
• Secondary research: 30 hours
• Interview: 3 doctors
• Survey: 3 potential patients, 2 doctors

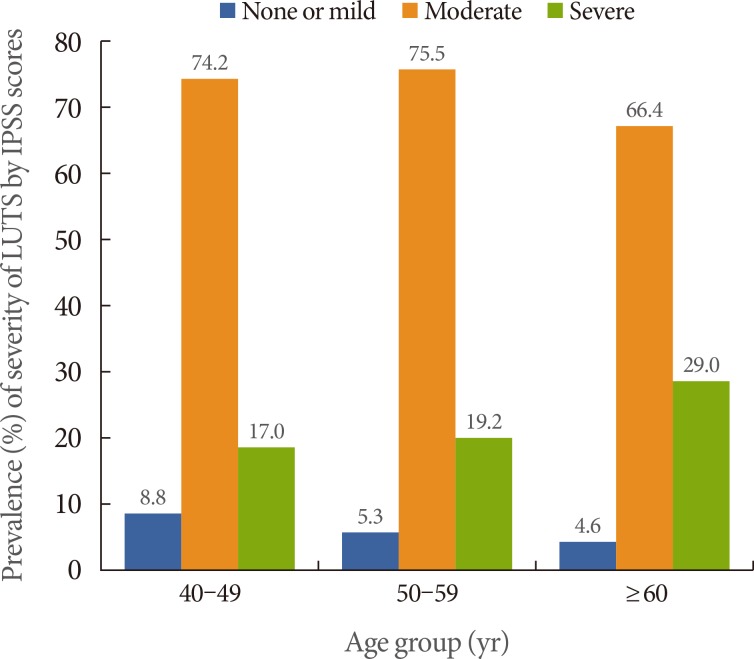
LUTS prevalence increases significantly with age
The prevalence of LUTS according to ICS criteria was 68.2% (men, 70.6%; women, 66.0%).
Symptoms can include:
Urinary incontinence, wanting to pass urine frequently, or experiencing pain or discomfort when you want to urinate.
Urology APP offers many benefits to LUTS patients and doctors
The app is simple and easy to use.
“Easy to use, just what I was looking for to track urology appointments.”
Easily keep track of daily urologic conditions.
“It keeps all the records for me and shows how the day-to-day changes.”
Saves time for clinic visits.
“It saved me a visit to the hospital.”
“Urologists are not going to spend their time answering all questions. It’s not worth the time to do it.”
LUTS patients are willing to pay
For example, iUflow (competing app) users pay $99 for the wireless and disposable uroflowmeter and bladder diary app.
Patients need to track uroflow regularly
Patients need to continuously record symptoms daily for treatment and prevention.
“I have been suffering from repeat UTIs and the doctor wanted me to monitor my urination frequency. So far, it’s been simple and easy to use.”
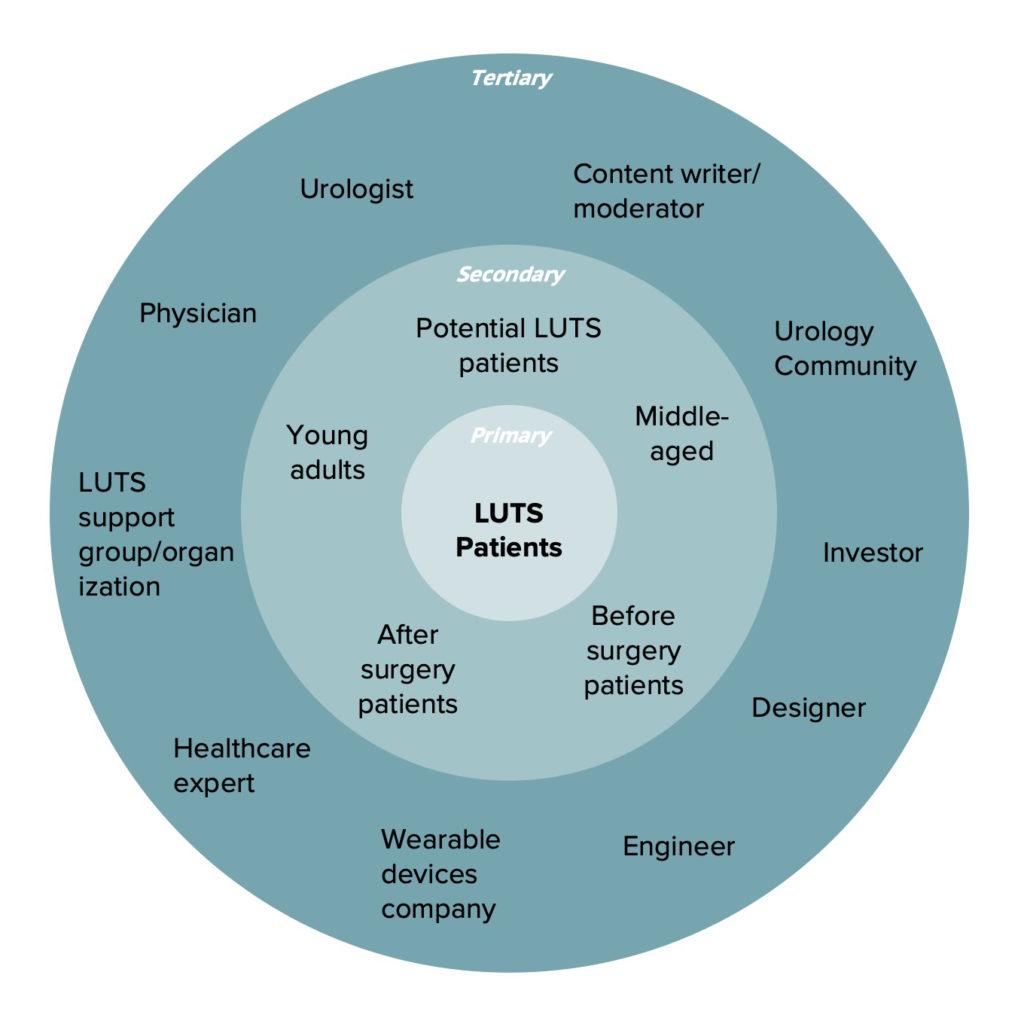
Stakeholder Map
Our primary stakeholders are Lower Urinary Tract Symptoms (LUTS) patients. The secondary stakeholders are potential patients as well as pre- and post-op patients. The tertiary stakeholders are mainly investors, the urology community, content moderators, engineers, and designers.
Key Findings
We analyzed our research and identified three key points. Current treatments take time and effort to track data. Patients with mild symptoms tend not to prevent or treat. The stigma of LUTS can make treatment embarrassing.
The current treatment requires a lot of effort in tracking data
Traditional LUTS uroflowmetry and voiding diary data collection are time-consuming and inefficient.
Early Prevention is often ignored
The current LUTS patients tend not to prevent or treat their conditions unless they have obvious symptoms.
Many patients with mild symptoms choose not to see a doctor. However, many early symptoms of LUTS can be prevented or delayed depending on people’s daily behaviors.
LUTS stigma makes people feel ashamed to seek help
LUTS patients often choose not to talk about their concerns or seek help. They feel embarrassed to talk about their urology concerns/symptoms. As a result, they miss the best window of time for treatment.
“The father wanted to talk about his concern with me privately without his son in the room.”
User Segments
We have identified three user segments. The first is surgical patients who need to keep urinary records. The second is people with high-risk symptoms. The third is those who want to know about urology.

LUTS patients before surgery and after surgery
Need to have the clear uroflow/voiding diary data and show it to urologists.
“I need help to track info for my doctor, something easier than pen and paper, and also reminds me to track my urine condition.”

High-risk LUTS people who want to prevent disease
Need to track and be careful about daily behaviors, and build certain habits to keep their bladder healthy.
“Many women have difficulties with bladder control after childbirth. I hope I can track urination and see behavioral patterns that can lead to increased bladder control.”

Young and middle-aged adults with mild urinary issues
Want to learn more and find support in the LUTS area
“If it could help me to figure out why I keep waking up at night to pee, that would be great.”
Solution
Create a Urology Community
Starting from the person who just needs to track their bladder health down to the person who wants to learn more about improving their urinary health, there are potential and diverse needs beyond the patient. We provide resources like articles, videos and chat rooms to encourage healthy, anonymous discussions around bladder control and urinary health in general.
For the first stage, we would like to focus on fine-tuning the bladder health tracker.
Next, we hope to expand and create more value for our customers by providing them with useful behavioral recommendations.
Finally, we aim to create medical content and build a urology community within our app to share about managing their urinary health.
Usage-based price model
Our business model is subscription-based and takes advantage of the freemium upsell. What this means is that we offer our product for 30 days, after which we start charging our users per month. Users can also choose from multiple pricing models for each usage range.
Purpose Statement
Our purpose is to provide an online platform for urology patients and potential patients so that they can easily understand and efficiently manage their bladder health at home.
Strategic Planning
We created a five-year roadmap and business model canvas for expanding app use, approaching it in three waves, and finally creating the urology information-sharing community.
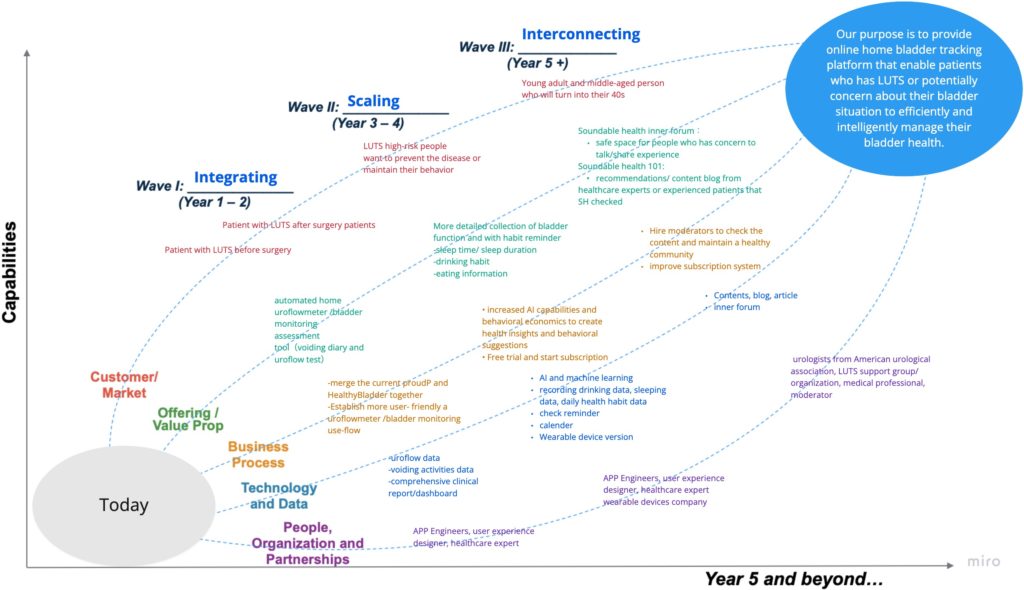
Strategy Roadmap
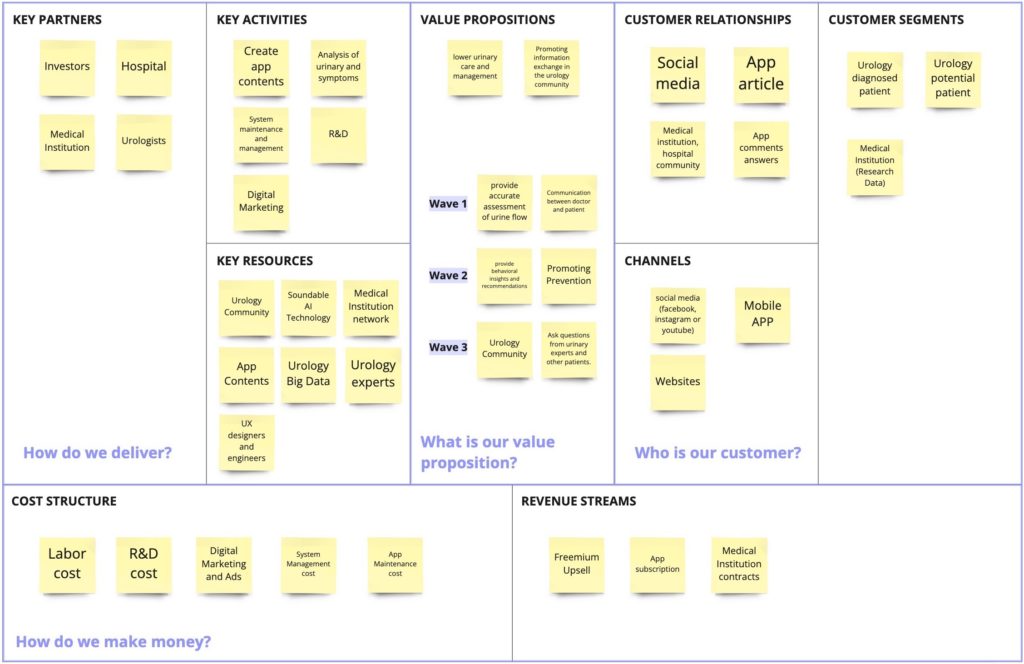
Business Model Canvas
Wave 1 – Integrating
Integrate the complicated functions, and allow patients to easily and comprehensively measure their urinary status at home before and after surgery and export data to the urologist.
Wave 2 – Scaling
Expand the functionality, and provide AI-based suggestions for behavioral improvements for people who are concerned about their bladder behavior. Record habits such as drinking and sleep, and adding calendar and reminders.
Wave 3 – Interconnecting
Create urology content and blogs to engage a wider range of users such as young adults and middle-aged people, and form an informative and trustworthy urology community.
Prototyping
Information Architecture
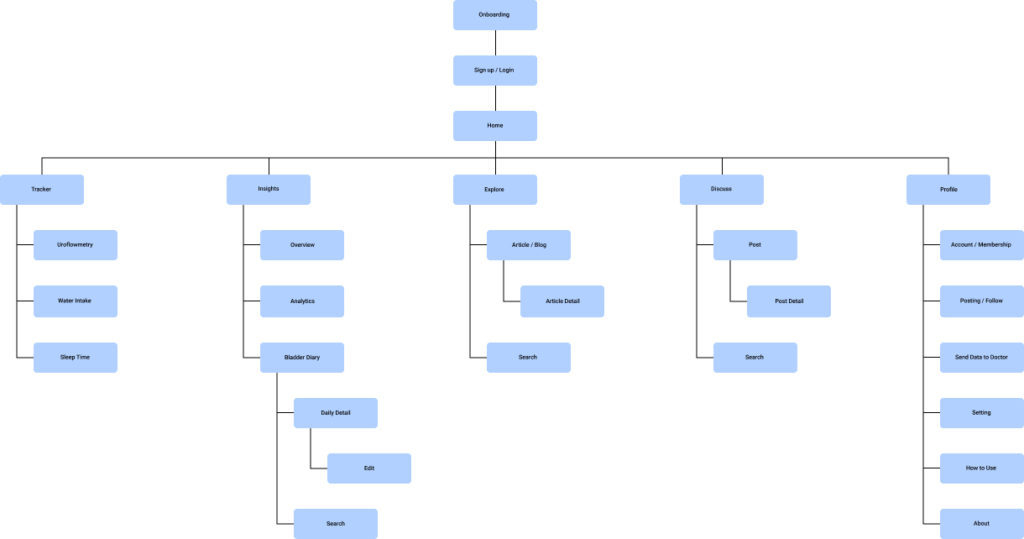
User Flow

Wireframe
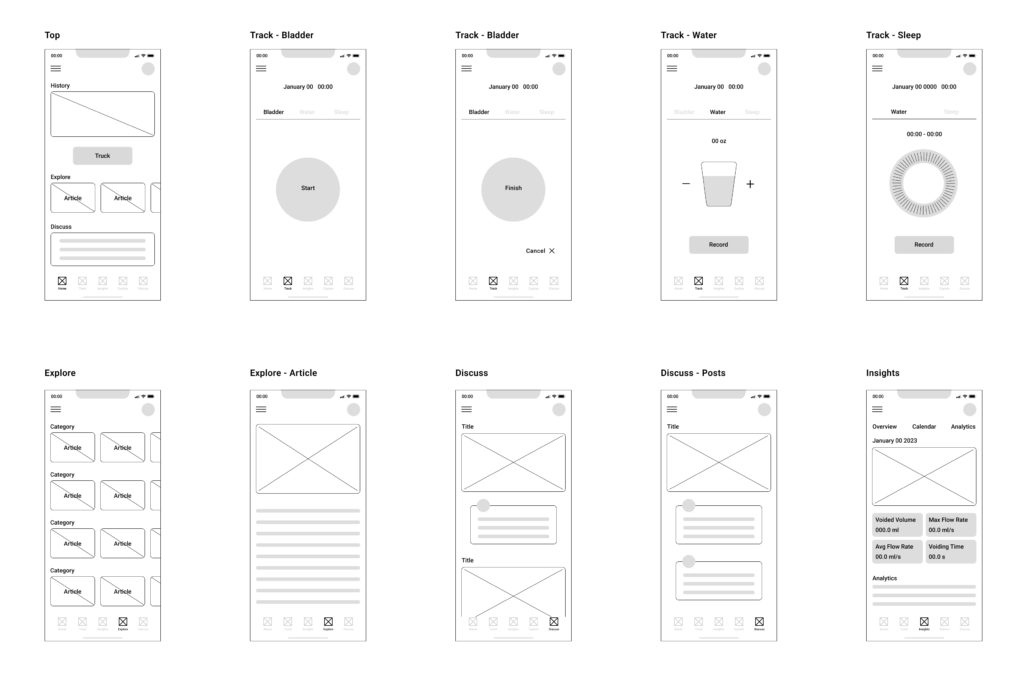
Prototype
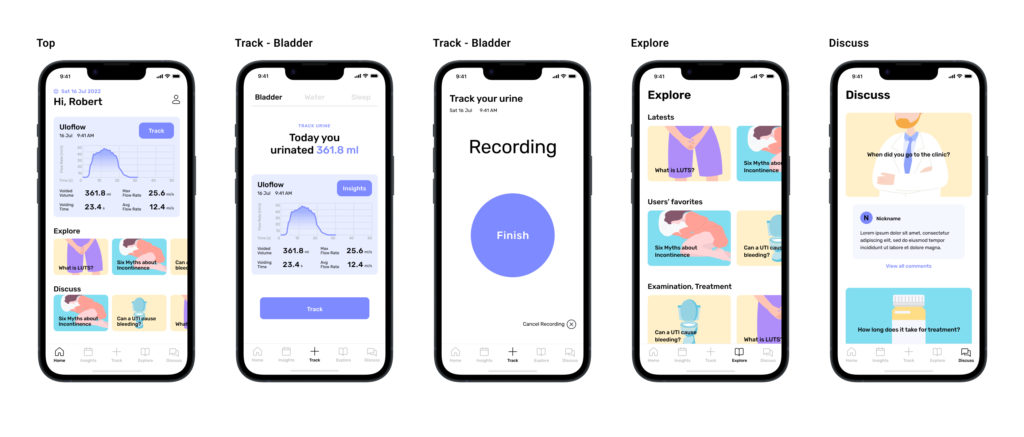
Next Steps
In-depth research with patients
Conduct in-depth research following human-centered design to identify necessary and unnecessary features and organize an appropriate service experience.
Collaboration with diverse stakeholders
Involve diverse stakeholders; not only patients and urologists, but also people experiencing mild symptoms, content creators, engineers, and service designers
Interview non-patients concerned about symptoms
Explore the needs and insights of potential patients and research what kind of information and community is appropriate to encourage prevention.